Every so often, a leading brand reminds us that true innovation in health and wellness begins with asking the right questions rather than riding the latest trend. GNC has done just that by undertaking the first real-world nutritional analysis of GLP-1 agonist users, a pioneering effort that promises to reshape supplement formulation, clinical guidance and patient education for healthcare professionals.
Bridging Clinical Trials and Daily Diet
GLP-1 receptor agonists such as semaglutide have transformed weight-management protocols, delivering remarkable results in controlled clinical trials. Yet those trials rarely reflect the complexities of everyday life – the hurried breakfast, the skipped snack, the reliance on convenience that comes with diminished appetite. Dr Brittany Johnson, PhD, RDN and Senior Manager of Scientific Affairs at GNC, recognized early on that formulating a support product without understanding real-world eating habits would risk missing the mark entirely. As she explains, “We set out last year to develop a product tailored to the unique needs of GLP-1 users. However, we quickly realized there simply wasn’t enough evidence to inform a formula based on our scientific standards.”
By choosing to investigate true eating habits rather than rely on assumptions, GNC differentiates itself in a market awash with speculative claims. This commitment to data over conjecture sets a new benchmark for evidence-driven wellness retail.
Methodology
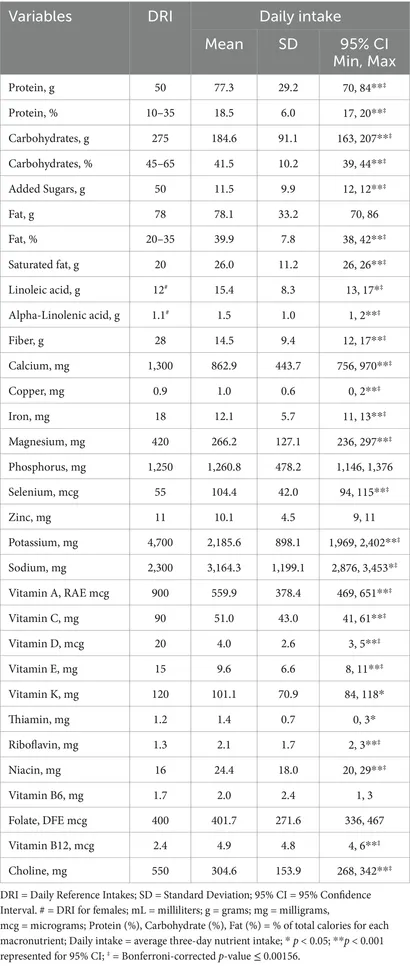
GNC’s study, Investigating Nutrient Intake During Use of Glucagon-like Peptide-1 Receptor Agonist: A Cross-Sectional Study, enrolled sixty-nine adults who had been on stable GLP-1 therapy for at least eight weeks. Participants logged every morsel and sip over a representative three-day period, noting portion sizes, preparation methods and mealtime contexts. This rigorous dietary survey was paired with validated nutritional analysis software to calculate macronutrient and micronutrient intakes. To assess protein adequacy, intake was expressed not only as a percentage of total calories but also in grams per kilogram of body weight, offering a body-weight-adjusted perspective that is vital for maintaining lean mass. Data accuracy was assured through double-entry coding and independent review by registered dietitians, eliminating common pitfalls of under- or over-reporting.
Such granularity – capturing everything from the fibre in a handful of berries to the calcium in a side of steamed broccoli – reveals a far more nuanced picture of how appetite suppression influences nutrient intake beyond simple calorie counts.
Shortfalls Among GLP-1 Users
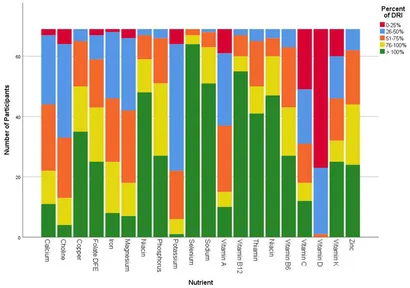
The results were both illuminating and concerning. Participants consistently failed to meet recommended servings for fruits, vegetables, whole grains and dairy, falling well below UK Public Health England and USDA MyPlate guidelines. Though total fat and saturated fat provided an excessive proportion of daily energy, this likely reflects a tendency to opt for higher-fat convenience foods when appetite re-emerges sporadically.
Most striking was the finding that mean protein intake, while accounting for 15–20 per cent of total calories, translated to only 0.6 grams per kilogram of body weight, significantly under the 0.8 g/kg threshold recommended for preserving muscle mass and metabolic health. Without sufficient protein, patients risk losing lean tissue, which can undermine both functional capacity and long-term metabolic control.
Micronutrient analysis revealed substantial deficits in fibre, calcium, iron, magnesium, potassium, choline and the antioxidant vitamins A, C, D and E. Such deficiencies have far-reaching implications, from compromised bone density and immune resilience to impaired recovery from exercise and reduced antioxidant defence. In short, the very therapy that delivers critical metabolic benefits could inadvertently create new nutritional vulnerabilities if left unaddressed.
Translating Findings into Strategies
Rachel Jones, MS, RDN and GNC’s Chief Merchandising & Science Officer, emphasizes that “science is the foundation for everything we do at GNC.” Armed with concrete evidence of nutrient shortfalls, practitioners can now recommend tailored interventions rather than generic advice. Clinicians and dietitians will be able to integrate body-weight-adjusted protein targets and specific micronutrient monitoring into routine therapy reviews, ensuring that patients receive personalized nutrition plans alongside their prescriptions.
On the product side, GNC is already leveraging these insights to refine its GLP-1 support programme. Future supplement formulations will be designed to plug the precise gaps identified – for example, a protein-fortified shake enriched with calcium, magnesium and vitamin D to support bone health and immune function. Educational materials, from meal-planning guides to digital recipe libraries, will spotlight nutrient-dense foods that help patients meet targets without overwhelming their reduced appetites. Rather than treating side effects like nausea or fatigue in isolation, GNC’s approach will address the root cause: suboptimal nutrient intake.
Charting the Path
For health industry professionals – whether in practice, research or product development – GNC’s real-world analysis signals a clear imperative: supplement innovation must be as evidence-based as the therapies it seeks to support. Pharmaceutical companies and wellness retailers alike should forge partnerships to conduct post-marketing surveillance on nutrient status among GLP-1 cohorts, creating a continuous feedback loop that refines clinical guidelines and product portfolios in real time. Regulatory bodies may also look to these findings when considering labelling requirements and health claims for support supplements, emphasizing the need for transparency and substantiation.
Looking ahead, GNC plans to expand its research to larger, more diverse populations and to explore intervention trials that assess the impact of targeted supplementation on clinical endpoints such as bone density, metabolic biomarkers and patient-reported quality of life. By demonstrating that robust science can underpin credible, consumer-centric solutions, GNC is not only raising the bar for supplement retailers but also equipping healthcare professionals with the tools they need to safeguard patient health in the era of GLP-1 agonist therapy.